9 Tips for Prioritizing Behavioral Health in the Workplace

Though mental health issues were prevalent before 2020, the pandemic made things significantly worse. From January to June 2019, 11% of U.S. adults reported symptoms of anxiety and/or depression. In January 2021, just under a year after the pandemic began, that number jumped to 41% — almost a 300% increase.
Unfortunately, while mental health issues have skyrocketed, care for behavioral health concerns has not. In fact, Castlight data show that starting March 2020 there was a steep decline in the rate of office-based psychiatric services, which includes psychotherapy, psychiatric diagnostic services, and psychiatric therapeutic services. Though telehealth utilization did increase dramatically during the pandemic, it wasn’t enough to fully offset the rising behavioral concerns and lack of in-person care, nor was the rise in telemedicine use equitable across different populations.
As the world opens up again and employers continue to figure out how to navigate the “new normal”—and help their employees do the same—prioritizing behavioral health is a must.
In a recent Castlight webinar, Susan Wyatt, head of Customer Success at Lyra Health, Dr. David Grodberg, chief medical officer at Brightline, and Mary Cain, senior director of Clinical Strategy and Behavior Change at Castlight, discussed the widespread impact of COVID-19 on behavioral health and how to best support employees in the workplace. Here are nine tips from the webinar.
Returning to Work: 9 Ways to Prioritize Behavioral Health
1. Listen to Your Employees.
It’s critical to make employees an active part of the return-to-work conversation. Consider conducting surveys and encouraging managers to solicit thoughts and suggestions from their teams. Help employees feel supported and that their voices are heard and valued by acknowledging their thoughts and concerns, asking what they need help with, and figuring out the best ways to support them.
2. Communicate Clearly, Frequently, and with Empathy
Though the pandemic is still evolving, “that shouldn’t stop you from communicating with your employees,” Wyatt says. “Because when you don’t, they fill in the gaps—sometimes with things that will ultimately drive more stress and anxiety.” Update your team as often as possible and make ample time for them to ask questions. Remember: Clear communication is kind.
3. Offer Benefits and Flexibility to Help Ease the Transition
Millions of employees across the country are struggling with the transition back to in-person operations, but not all for the same reason. Some are nervous about commuting, some don’t have child care anymore, some are worried their productivity will plummet once they’re back in the office. The point is, every situation is different, and your employees will need support and understanding in order to navigate the transition—and beyond. “As much as you can, offer flexibility as we make this transition,” Wyatt says. “And make sure you’re reminding everyone about the benefits you have to support them wherever they’re at.”
4. Empower Your Leaders to Lead by Example
Your leaders—executives and middle managers—are responsible for setting an example and driving company culture. As such, they should model the same behaviors you want all employees to engage in, such as taking time off and using benefits programs. When employees see leadership take care of themselves, they feel more comfortable doing the same.
At Lyra Health, a comprehensive mental health provider, Wyatt says the customers with the highest levels of engagement are the ones in which senior leaders openly talk about mental health. “Not just from a benefits perspective,” Wyatt says, “but their experience with it and why it’s important.”
In addition, consider training all people managers to recognize some of the main symptoms of mental health struggles like anxiety and depression and how they can best intervene.
5. Ensure Multidisciplinary Care Teams
Comorbidities are common in behavioral health, and this is especially true among children and adolescents. For example, 60% of kids with ADHD have at least one other behavioral health condition. That usually means parents have to drive around town to see multiple providers who aren’t always working together on a shared clinical record. By investing in multidisciplinary teams, benefits leaders can offer both more convenient and better quality care. “This approach allows for improved care coordination, the right treatment sequencing, and a better overall experience for your employees,” Grodberg says.
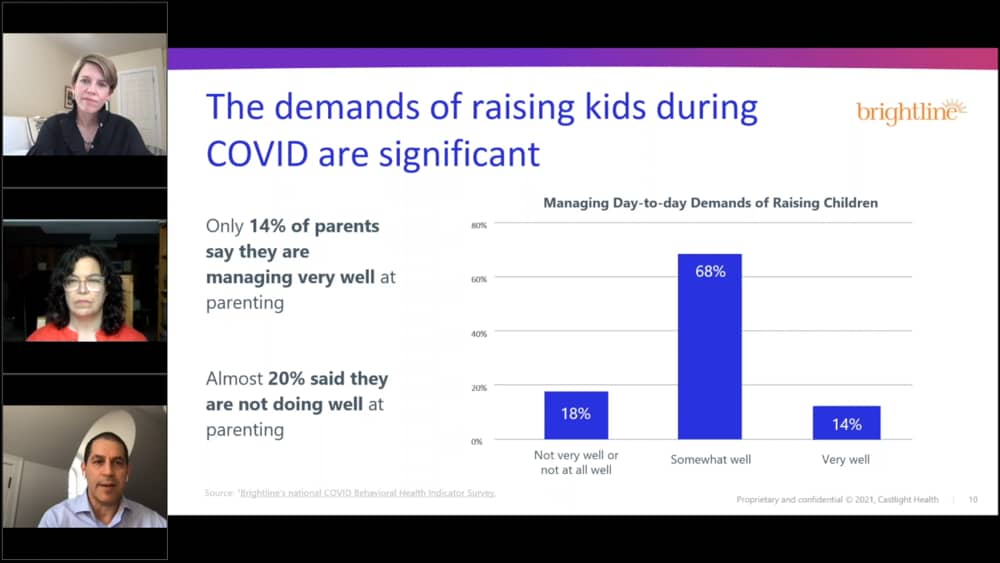
6. Provide Family-Centered Care
Research indicates that parents of kids with depression are 50% more likely to suffer from depression themselves. As a benefits leader, it’s wise to invest in a family system of care that works with both parents and kids. “Now more than ever,” Grodberg says, “care needs to be personalized and truly family-centered.” In addition, parents should be able to tailor care to their wants and needs. “If for whatever reason, they’re not ready to enter [their child into] clinical care, there needs to be a solution that allows them to access care like group or child-focused coaching in order to get engaged.”
7. Centralize Access to All Health Resources
Providing one, single place employees can visit to access all their different health benefits resources is key, as you want it to be as simple as possible for them to find what they need and engage regularly. The fewer links, apps, and passwords they have to keep track of, the better.
8. Identify and Engage Vulnerable Groups
People don’t always have a behavioral health diagnosis, but that doesn’t mean they’re not struggling. It’s very likely most of your employees are dealing with some sort of stressors that are making it harder for them to focus and be productive at work. Figuring out who is struggling and what they’re struggling with—whether you gather this information through surveys, one-on-one conversations, or search activity in a health navigation system—will help you personalize outreach and messaging (and thus increase engagement).
9. Provide Digital and High-Touch Navigation Support
Digital navigation solutions can help steer employees to the right care at the right time, but high-touch advocacy support—like Castlight Care Guides—is key to discovering unmet behavioral needs and closing more gaps in care. Often, when a clinically complex individual reaches out to a Care Guide for an entirely separate issue, the Care Guide uncovers a behavioral health concern. In most situations, the member isn’t aware of the issue or hasn’t sought support for it ever or in a while, and the Care Guide can connect them with the appropriate care.
“The need for pediatric and adult behavioral care has been a headline issue—literally, it’s been on covers of magazines and news stories—and I think that’s a welcome thing,” Grodberg says. But as employers move forward with the return to work and addressing behavioral health, Grodberg cautions, “The barriers to clinical care are still there, even though the drivers of need are much more. Whatever solution you come up with really needs to break down those barriers.”
To hear more about how employers can approach behavioral health, watch the webinar. To view all of our past webinars and register for upcoming webinars, click here.


